PCOS Symptoms, Diagnosis, and Treatment Options
Polycystic Ovary Syndrome (PCOS) affects nearly 1 in 10 women of reproductive age, according to the
World Health Organization.
Because PCOS involves significant hormonal imbalance, it can influence menstrual cycles, ovulation, metabolism, weight, and overall fertility.
However, early diagnosis and the right treatment plan can dramatically improve long-term health outcomes.
This expert-backed guide explains PCOS symptoms, diagnosis, and treatment options.
It also includes insights commonly shared by gynecologists and PCOS specialists in Panchkula, Chandigarh, Mohali, and Dera Bassi, ensuring clarity and medical accuracy.
Home – Dr. Nitasha Gupta
About – Dr. Nitasha Gupta
Book Appointment
Google Business Profile – Dr. Nitasha Gupta
Kore Fertility Solutions – GMB Listing
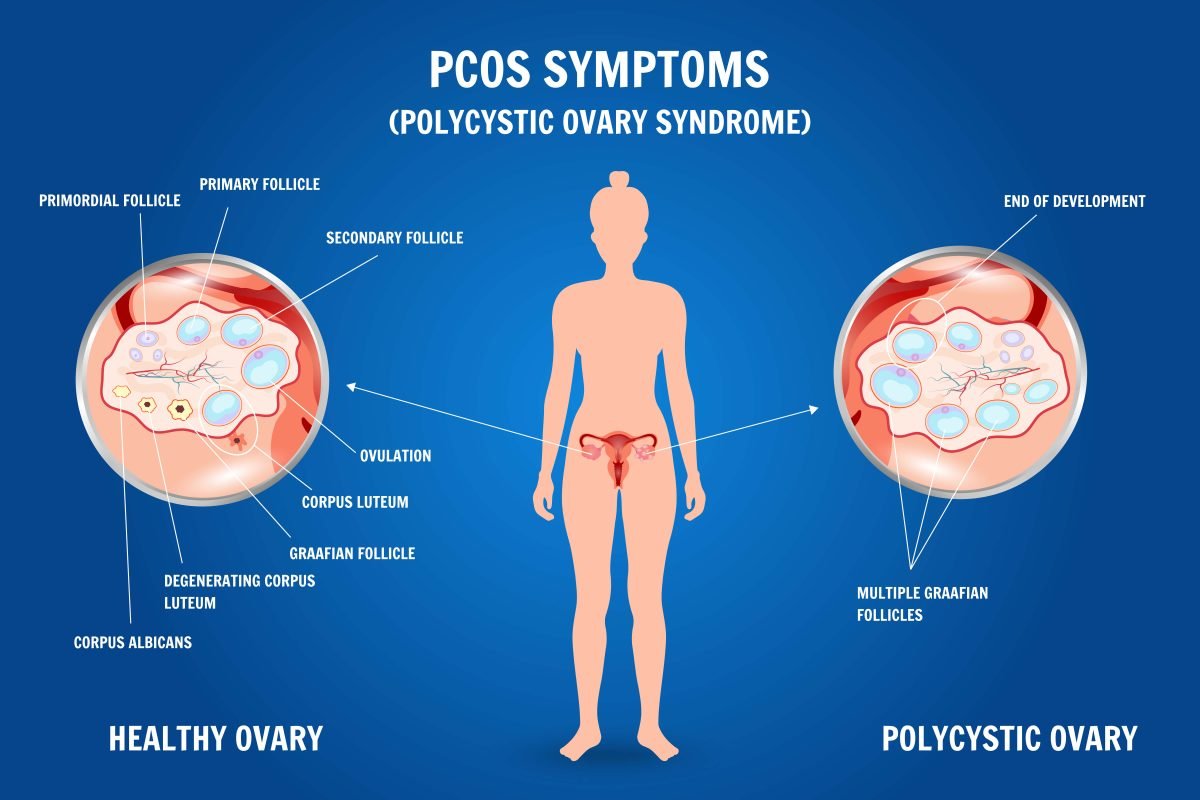
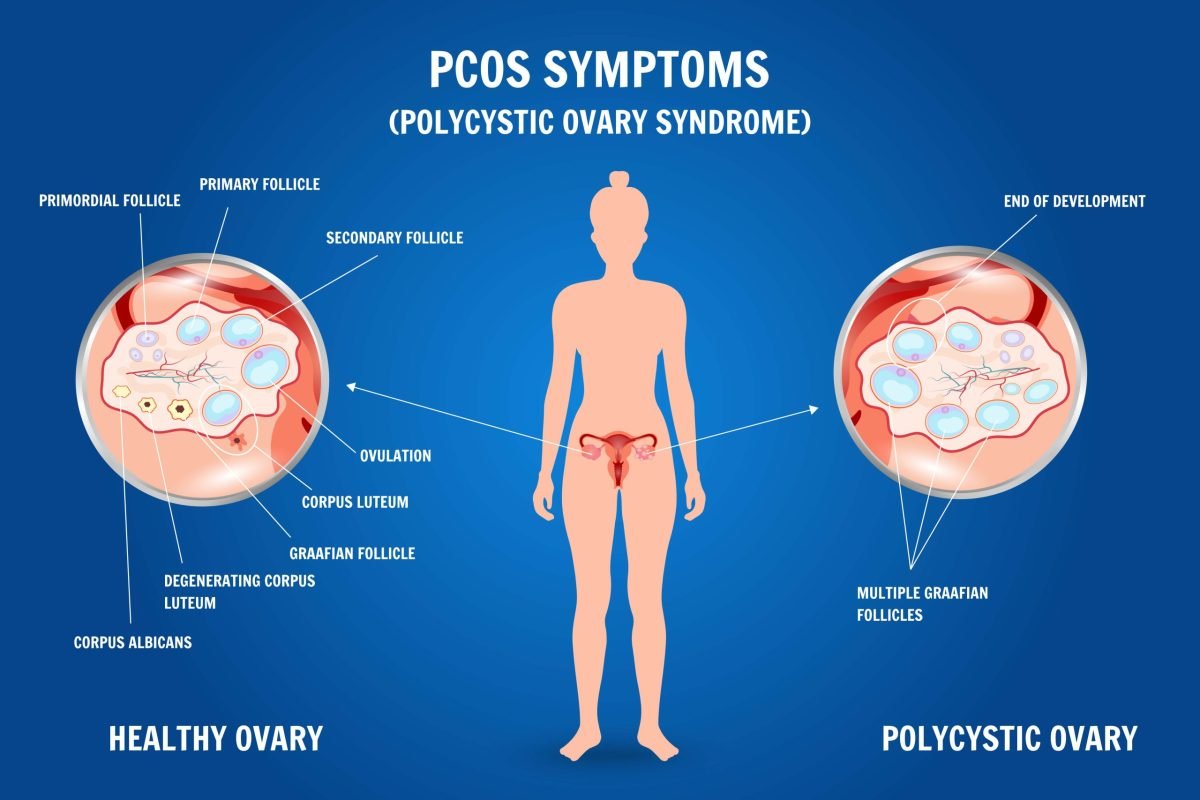
What Is Polycystic Ovary Syndrome (PCOS)?
PCOS occurs when the ovaries produce excessive androgens—hormones normally present in women in small amounts.
Because these elevated hormones disrupt egg development and ovulation, several symptoms begin to appear gradually.
Due to hormonal imbalance, many women notice changes such as:
- Irregular menstrual cycles
- Cystic-appearing ovaries
- Difficulty conceiving
- Acne and unwanted hair growth
- Insulin resistance and metabolic issues
Although PCOS is often misunderstood, ovarian cysts are not required for diagnosis.
In fact, PCOS is primarily a hormonal and metabolic condition rather than a structural one.
Common Symptoms of PCOS
Because PCOS affects each woman differently, symptoms can range from mild to severe.
Irregular Periods
Cycles may become longer than 35 days, fewer than eight per year, or absent for months due to irregular ovulation.
Excess Androgen Levels
High androgen levels may lead to:
- Facial or body hair growth (hirsutism)
- Severe acne
- Scalp hair thinning
Polycystic Ovaries
Small, immature follicles line the ovaries, often appearing as a “string of pearls” on ultrasound.
Infertility
Because ovulation becomes irregular, PCOS is one of the most common causes of infertility.
Fortunately, many women conceive with proper ovulation induction or fertility treatments like
IUI or IVF.
Weight Gain & Insulin Resistance
PCOS often causes abdominal weight gain due to insulin resistance.
Over time, this may increase the risk of type 2 diabetes, especially without intervention.
Emotional & Mental Health Symptoms
- Mood swings
- Anxiety
- Depression
- Disturbed sleep
Diagnosis of PCOS
Diagnosing PCOS requires a combination of medical history, physical examination, and diagnostic testing.
Because symptoms overlap with other hormonal disorders, accurate testing is essential.
1. Medical History Review
Doctors discuss menstrual patterns, skin concerns, hair changes, weight shifts, and family history.
2. Physical Examination
Visible signs such as acne, hair growth, or obesity may indicate hormonal imbalance.
3. Ultrasound
A pelvic ultrasound helps identify enlarged ovaries or multiple small follicles.
4. Blood Tests
Common tests include:
- Testosterone
- LH/FSH ratio
- Fasting insulin
- Thyroid panel
- Prolactin
Rotterdam Criteria:
A diagnosis requires 2 out of 3 features:
- Irregular ovulation
- High androgens
- Polycystic ovaries
Treatment Options for PCOS
Although PCOS has no permanent cure, its symptoms can be managed successfully with lifestyle changes, medication, and supportive therapies.
With proper treatment, most women lead completely healthy lives.
Lifestyle Modifications
Healthy Diet: A nutrient-balanced, low-GI diet improves insulin sensitivity. Recommended options include:
- Whole grains
- Protein-rich foods
- Green vegetables and fruits
- Nuts and seeds
- Low-glycemic carbohydrates
Regular Exercise: Cardio plus strength training improves insulin response and supports weight control.
Medications
Birth Control Pills: Used to regulate cycles and reduce androgen levels.
Metformin: Helps manage insulin resistance and may regulate ovulation.
Anti-Androgens: Medicines like spironolactone reduce excessive hair growth and acne.
Fertility Medications
For women trying to conceive, doctors may prescribe:
- Letrozole
- Clomid (clomiphene)
- Gonadotropin injections
Hair Removal Treatments
Treatments like laser and electrolysis provide longer-term results for androgen-related hair growth.
Surgical Option: Ovarian Drilling
A laparoscopic procedure that reduces androgen-producing tissue, helping restore ovulation in selected cases.
Mental & Emotional Support
Therapy, mindfulness, and counseling help women manage stress, emotional fluctuations, and sleep disturbances caused by PCOS.
When to Consult a PCOS Specialist in Panchkula, Chandigarh, or Mohali
- Irregular or absent periods
- Unwanted facial or body hair
- Severe acne
- Rapid weight gain
- Fertility difficulties
- Signs of hormonal imbalance
Mayo Clinic – PCOS Overview
CDC – PCOS Information
NCBI – PCOS Research
WHO – Women’s Health
Conclusion
PCOS is a multifaceted hormonal and metabolic disorder, yet it is highly manageable with timely evaluation and the right treatment plan.
Because early lifestyle changes and proper medications significantly reduce long-term risks, consulting an experienced gynecologist is essential.
If you’re experiencing symptoms such as irregular cycles, acne, weight gain, or fertility challenges, book a consultation with a
PCOS specialist in Panchkula, Chandigarh, or Mohali
for personalized and effective treatment.
Frequently Asked Questions (FAQs)
Q1. Can PCOS be cured?
No. Although PCOS cannot be permanently cured, its symptoms can be effectively managed.
Q2. Does PCOS always cause infertility?
No. Many women conceive naturally or with the help of fertility treatments.
Q3. Should every woman with PCOS get an ultrasound?
Not always. Diagnosis depends on symptoms, blood tests, and clinical patterns.
Q4. Can lean women have PCOS?
Yes. Thin women can also experience hormonal imbalance and irregular ovulation.
Q5. Is PCOS genetic?
Yes. Family history often increases the risk.
Q6. Does PCOS increase diabetes risk?
Yes. Insulin resistance makes women more prone to type 2 diabetes.